How to Read IVF Success Rates: What Patients Should Actually Look At
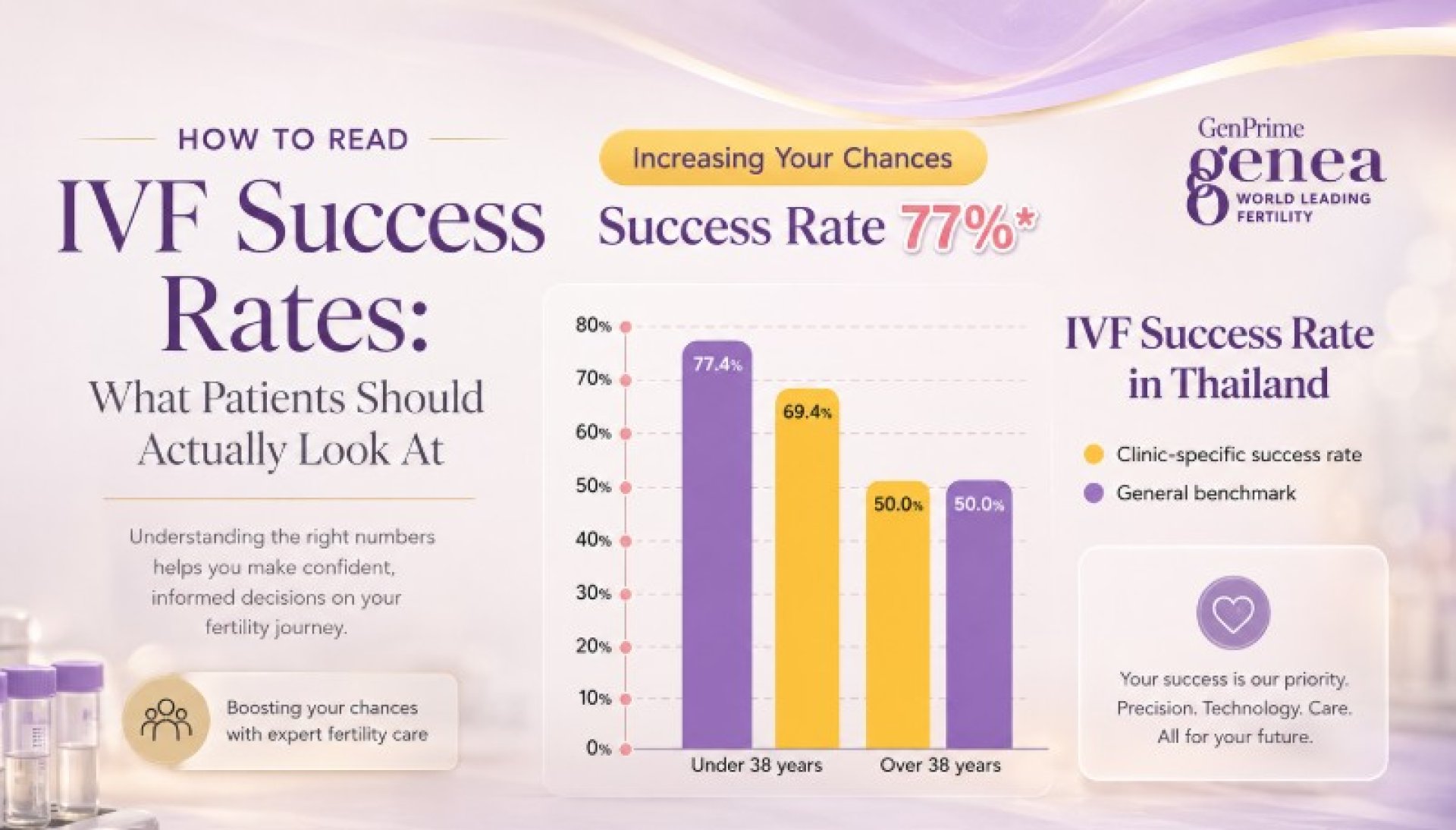
When researching IVF clinics, many people quickly encounter numbers such as:
- “70% success rate”
- “high pregnancy rate”
- “top IVF outcomes”
At first glance, these figures may seem straightforward. But in reality, IVF success statistics are often more complex than they appear. Different clinics may measure outcomes differently, report different patient groups, or focus on different stages of treatment. Because of this, comparing IVF clinics based only on a single percentage can sometimes be misleading.
Understanding what IVF success rates actually mean, and how to interpret them in context, can help patients make more informed decisions when exploring fertility treatment.
What Does “IVF Success Rate” Actually Mean?
One of the most important things to understand is that there is no single universal definition of “IVF success rate”. Different clinics may report different types of outcomes, including:
- positive pregnancy tests
- clinical pregnancies confirmed by ultrasound
- ongoing pregnancies
- live births
These are not identical outcomes, and they occur at different stages of the IVF journey. For this reason, when patients compare IVF statistics, it is important to understand which outcome is actually being measured.
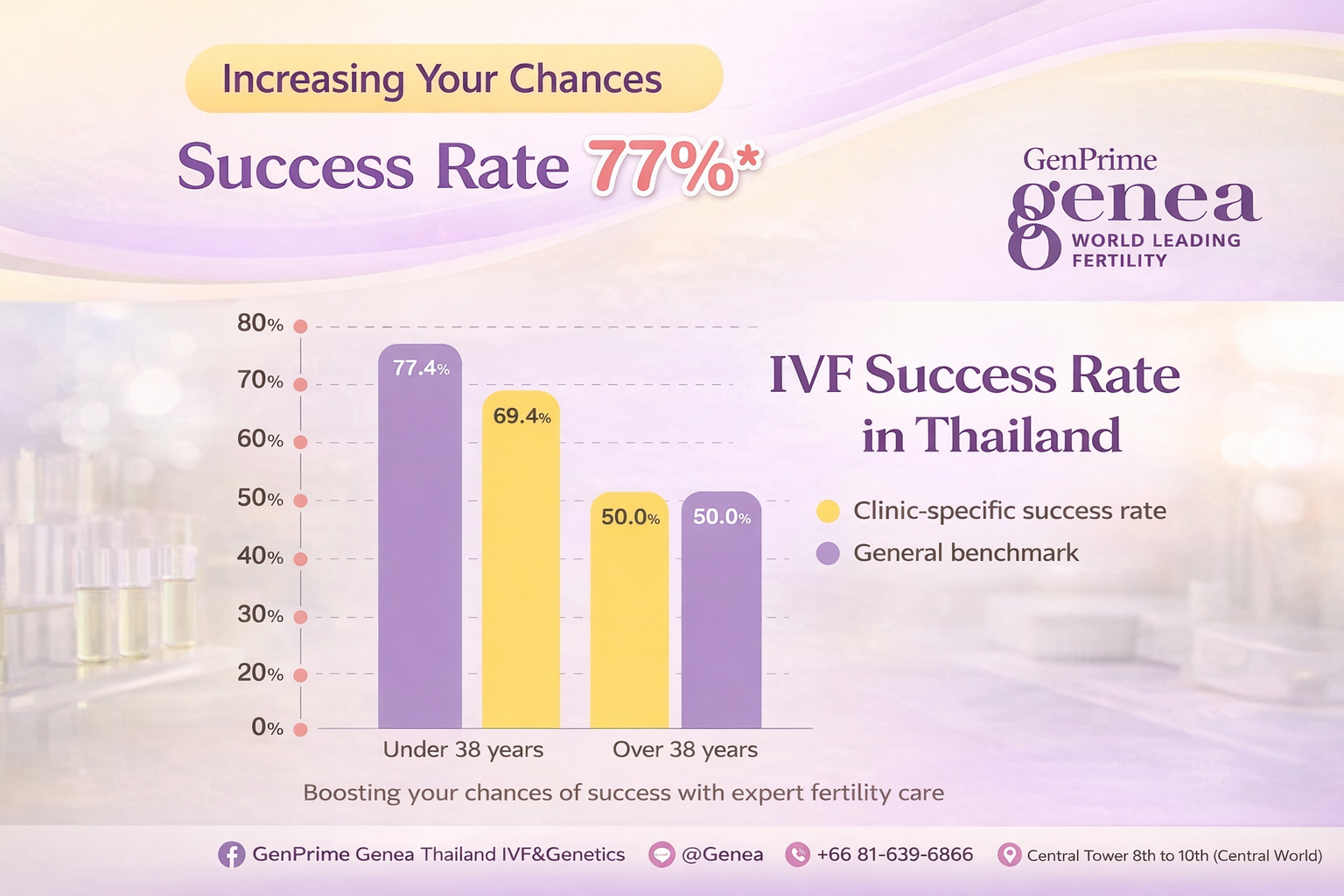
Pregnancy Rate vs Live Birth Rate
A positive pregnancy test is usually one of the earliest signs that implantation has occurred. This is often referred to as a biochemical pregnancy. A few weeks later, an ultrasound may confirm the presence of a gestational sac or fetal heartbeat, which is typically referred to as a clinical pregnancy.
However, from a patient perspective, many specialists consider live birth rate to be one of the most meaningful long-term outcome measures, because it reflects the final outcome of treatment rather than an earlier stage of pregnancy. This does not mean that earlier milestones are unimportant. Rather, it highlights why different success statistics may tell different parts of the same story.
Why Age-Specific Data Matters
Age is one of the most important factors influencing IVF outcomes. Because egg quality and chromosomal normality tend to change over time, IVF success rates are often very different between age groups. For example, outcomes for patients under 35 may differ significantly from those for patients aged 40 or above.
This is why overall clinic averages can sometimes be difficult to interpret without additional context. When reviewing IVF statistics, patients may find it helpful to look for information that is broken down by age group rather than relying only on overall percentages.
Why Different Clinics May Report Different Numbers
IVF success rates can vary between clinics for many reasons. These may include:
- differences in patient age profiles
- whether more complex cases are accepted
- differences in reporting methods
- variations in laboratory systems and clinical protocols
- whether statistics refer to fresh or frozen embryo transfers
IVF Success Is Not One Single Step
Another common misconception is that IVF success is determined by a single moment. In reality, IVF involves several stages, including:
- egg retrieval
- fertilisation
- embryo development during embryo culture
- blastocyst development
- embryo transfer
- implantation
- ongoing pregnancy
- live birth
At each stage, biological factors and laboratory processes may influence what happens next. Understanding IVF as a multi-step process can help patients better interpret why outcomes are not always predictable from the beginning of a cycle.

Why Embryo Development Matters
After fertilisation, embryos continue developing in the laboratory over several days. During this period, embryologists observe how embryos divide and progress through different stages of development. By around day five to six, some embryos reach the blastocyst stage, which is often considered suitable for transfer, freezing, or genetic testing.
Not all embryos will continue developing at the same pace, and this variation is a normal part of human reproduction. Because embryo development happens outside the body during IVF treatment, laboratory conditions and embryology expertise play an important role in supporting embryo culture.
Do Technologies Like Time-Lapse Monitoring Affect Outcomes?
Some clinics use technologies such as time-lapse embryo monitoring to continuously observe embryo development while embryos remain inside the incubator. This allows embryologists to review developmental patterns in greater detail without repeatedly removing embryos from stable culture conditions.
(Read more about how time-lapse embryo monitoring works: https://www.genea.co.th/blog/9282/how-advanced-ivf-laboratory-technology-supports-fertility-treatment )
Similarly, some patients may undergo preimplantation genetic testing (PGT), which provides additional genetic information about embryos before transfer.
(Learn more about PGT and when it may be considered: https://www.genea.co.th/blog/9312/what-is-pgt-genetic-testing-in-ivf-and-who-should-consider-it )
These technologies do not guarantee pregnancy or live birth. However, they may provide additional information that supports embryo assessment and treatment planning in selected situations.
Why Transparency Matters When Discussing IVF Outcomes
Because IVF treatment is emotionally and financially significant, many patients want clear and realistic explanations about what success statistics actually represent. This includes understanding:
- what type of outcome is being measured
- whether data is age-specific
- whether complex cases are included
- how treatment recommendations are made
Questions Patients May Consider Asking About IVF Success Rates
When comparing clinics or reviewing IVF statistics, some patients may find it helpful to ask:
- Does this statistic refer to pregnancy rate or live birth rate?
- Is the data broken down by age group?
- Are complex fertility cases included in these numbers?
- Does the clinic explain both benefits and limitations clearly?
- How are laboratory processes and embryo development monitored?
- Is treatment planning personalised to the individual situation?
Looking Beyond Numbers Alone
Success statistics are important, but they are only one part of fertility treatment. For many patients, other factors may also matter, including:
- how clearly information is explained
- whether treatment feels personalised
- how comfortable they feel with the clinic’s communication style
- whether they feel involved in decision-making
- how transparent the clinic is about uncertainty and limitations
GenPrime Genea’s Approach
GenPrime Genea’s approach to fertility care combines embryology, genetics, and clinical planning as part of an integrated IVF programme. Built on Genea’s 40 years of IVF and fertility expertise in Australia, GenPrime Genea combines advanced embryology and genetic testing to support individuals and couples on their fertility journey.
This includes the use of IVF laboratory technology, embryo culture systems, time-lapse monitoring, and genetic testing where appropriate, alongside a focus on personalised treatment and informed decision-making.

Frequently Asked Questions
Q: What is the difference between pregnancy rate and live birth rate in IVF?
A: Pregnancy rate may refer to an early positive pregnancy test or a clinical pregnancy confirmed by ultrasound. Live birth rate refers to the number of treatment cycles that result in a live birth, which many specialists consider one of the most meaningful long-term outcome measures.
Q: Why do IVF success rates vary between clinics?
A: Success rates may vary because clinics treat different patient populations, use different reporting methods, and manage different levels of case complexity. Laboratory systems and treatment approaches may also differ.
Q: Do advanced IVF technologies guarantee better outcomes?
A: No technology can guarantee pregnancy or live birth. Technologies such as time-lapse monitoring or genetic testing may provide additional information that supports embryo assessment and treatment planning, but outcomes still depend on many biological factors.
Q: Why do some embryos stop developing during IVF?
A: Not all embryos continue developing to the blastocyst stage. This can be influenced by factors such as egg quality, sperm factors, chromosomal variation, and natural biological processes.
Q: What should patients focus on when comparing IVF clinics?
A: In addition to success statistics, patients may consider laboratory quality, embryology expertise, communication style, transparency, personalised treatment planning, and whether the clinic explains both benefits and limitations clearly.


